Vaginal Estrogen Guide: Which Suppository to Use

If you’re dealing with menopause symptoms like vaginal dryness, painful sex, and frequent UTIs, you may be considering vaginal estrogen therapy. Vaginal estrogen is a safe, effective treatment (delivered as a vaginal cream, ring, insert, or tablet) that can restore healthy function to your vulva, vagina, and urinary tract. Research shows this treatment can quickly improve some common and troublesome symptoms of menopause. Here’s what you should know about vaginal estrogen medication.
Why do people take vaginal estrogen?
Estrogen is one of the most important hormones you make. Almost every part of your body responds to it, including your heart, muscles, bone, brain, and skin. During menopause, your body’s production of natural estrogen decreases. This decline in estrogen levels triggers a cascade of changes throughout your body. Your vulva, vagina, bladder, and pelvic muscles (which are especially rich in estrogen receptors) are no exception.
This leads to one of the most common and distressing menopause symptoms—a cluster of issues called the genitourinary syndrome of menopause (GSM). GSM involves a short list of problems familiar to many people during menopause:
- Dryness, irritation, and itching of the vagina and vulva
- Pain and/or bleeding during sex
- Less sexual lubrication
- More frequent urinary tract infections
- Frequent need to urinate
- Pain or burning sensation while urinating
Vaginal hormone therapy eases these symptoms by delivering estrogen directly into the tissues that need it, helping restore their normal function. Research has proven that this therapy is effective. A 2019 review found that vaginal estrogen helps reduce vulvovaginal atrophy (i.e. the thinning and weakening of the vagina that can cause painful sex and irritation), improve overactive bladder (which causes frequent urination), and protect against urinary incontinence.
How does vaginal estrogen work?
Vaginal estrogen medication is available as a tablet, cream, or ring. Both the tablet and the cream are inserted into the vagina with a special applicator. This is typically performed daily for the first few weeks, and several times weekly thereafter. A ring, on the other hand, is inserted once and replaced every 90 days. The ring slowly releases a low dose of estrogen over this time period.
The tissues of your vagina are highly absorbent. When they begin receiving estrogen, almost immediate changes are triggered in your vaginal and urinary tissues. Estrogen causes the lining of your vagina (i.e. the epithelium) to thicken, making the tissue stronger, less fragile, and more elastic. It can also strengthen your pelvic floor muscles, helping improve urinary symptoms. In addition, estrogen seems to increase glycogen—a sugar that feeds healthy bacteria in your vagina, particularly Lactobacillus. This leads to positive changes in your vaginal microbiome, helping protect against urinary tract infections.
Is vaginal estrogen safe?
Vaginal estrogen is a safe and FDA-approved medication. The world’s foremost authority on menopause—the North American Menopause Society—has formally endorsed vaginal estrogen as a treatment for GSM. According to the group, vaginal estrogen is safe and effective for symptoms like vaginal irritation, pain during sex, and urinary issues.
For people with a history of cancer, there are special considerations around vaginal estrogen. Some forms of cancer are hormone-sensitive, meaning they grow in response to estrogen. (This is why many breast cancer survivors are prescribed estrogen blockers like tamoxifen.) In these cases, vaginal estrogen may still be a safe option under the care of a medical professional. The American College of Obstetricians and Gynecologists (ACOG) has stated that low-dose vaginal estrogen is an acceptable treatment option for cancer survivors, as long as the patient and doctor carefully weigh the risks and make a shared decision.
Vaginal estrogen, like other forms of hormone therapy, is best for people who are perimenopausal or have recently entered menopause. If many years have passed since you entered menopause, your doctor may find that the risks of vaginal estrogen therapy outweigh the benefits.
Who shouldn’t use vaginal estrogen?
Vaginal estrogen isn’t for everyone. You should not use this treatment if you have certain medical conditions, including:
- A history of stroke or heart disease
- Breast cancer (now or in the past)
- Liver disease
- A history of blood clots or high risk for blood clots
- Endometrial cancer
- Gallbladder disease
What are vaginal estrogen suppositories?
Vaginal estrogen medication can be delivered in several different forms, including as a suppository—i.e., a vaginal insert that slowly releases estrogen. This estrogen can easily enter the walls of your vagina, which are rich in blood vessels and highly absorbent. Estrogen suppositories are typically made in tablet or gel caps form. They can be inserted by hand or with a plastic applicator made by the drug manufacturer.
Research suggests that estrogen suppositories are more effective than other drug delivery modes (such as oral estrogen and the transdermal estrogen patch) when treating vaginal dryness and painful intercourse. This is due to the fact that suppositories deliver estrogen exactly where it’s needed—in the vaginal tissues. They can also come with fewer side effects, as the total amount of systemic estrogen you’re exposed to is lower.
Practical concerns about estrogen suppositories
You might imagine that an estrogen suppository would simply slide out of your vagina. This is a common concern, but is almost never an issue for people using vaginal suppositories. That’s because the vagina doesn’t follow a straight up-and-down path. It curves toward the top, so the upper part of your vaginal canal is almost horizontal when you’re standing upright. In addition, the lining of the vagina has many small ridges called rugae. These folds give the suppository a surface to grip, preventing it from falling out. They also create an abundance of surface area which helps absorb the medication.
If you’re wary of inserting a suppository into your vagina simply because it could be uncomfortable, rest assured that the inserts are very small and easy to use. And for many people, they actually prove more convenient than oral estrogen pills, because they’re used less frequently. Some brands, for instance, are used just twice a week. This can be easier to keep up with than a daily oral estrogen pill.
How to choose a vaginal estrogen suppository
When it comes to vaginal estrogen suppositories, you have several options to choose from. These include Vagifem (an estrogen tablet), Yuvafem (a generic form of Vagifem), and Imvexxy (an estrogen gel-cap). If you’re comparing these brands, there are a number of factors to consider.
Both Vagifem and Yuvafem tablets require a disposable plastic applicator, which you might find to be wasteful or inconvenient. Imvexxy, on the other hand, is a smooth gel-cap that can be inserted by hand. Additionally, Vagifem and Yuvafem are only available in 10-microgram doses, while Imvexxy is available (and has been proven effective) in a 4-microgram dose. For people trying to avoid side effects or simply take the smallest possible dose of hormone therapy, this can be appealing.
On the other hand, Imvexxy tends to be significantly more expensive than both Vagifem. As a generic medicine, Yuvafem is the most affordable option of the three. And while Yuvafem is chemically identical to Vagifem, some people prefer the latter simply because it has better brand recognition.
Ultimately, there’s no one-size-fits-all answer here. You’ll need to chat with your healthcare provider about the available options and choose whichever you feel most comfortable with.
How to use estrogen suppositories
There are many brands of estrogen suppositories available, and different manufacturers offer different guidance on how to use their products. That’s why it’s important to read the instructions carefully and check in with your healthcare provider if you have any questions. But generally speaking, inserting a suppository is a quick, easy process following the steps below.
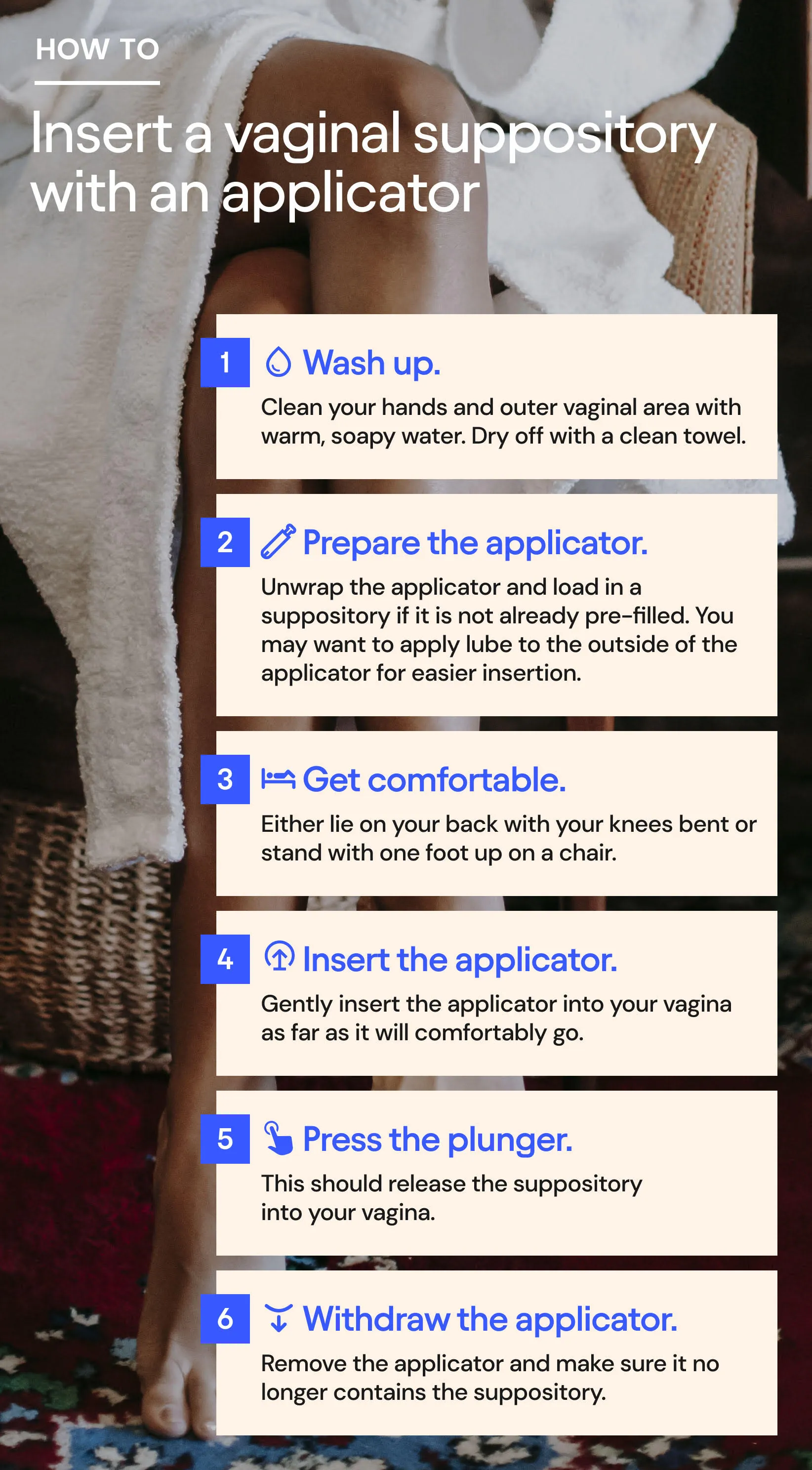
You’re done! You may need to remain lying on your back for a few minutes to allow the suppository to settle in. Dispose of the applicator as instructed or clean it if it’s meant to be reused.
Vaginal estrogen vs. other types of hormone therapy
If you’re interested in hormone therapy, vaginal estrogen is not the only option. Estrogen can also be taken orally (as a pill) or topically (as a cream or gel absorbed through your skin). Both of these approaches offer distinct benefits and are sometimes combined for optimal effect.
Oral estrogen therapy—i.e. swallowing a dose of estrogen in pill form—has been used longer than any other hormone therapy. For that reason, it’s the best-studied. We know that oral estrogen is effective at reducing the most common and troublesome symptoms of menopause: hot flashes and night sweats. It may also help with depression, insomnia, and mood changes. These are important benefits that you cannot always obtain with vaginal estrogen, which is why the two treatments are sometimes prescribed in combination.
On the other hand, estrogen taken orally has to first pass through your liver before it reaches your bloodstream and makes its way to your vaginal tissues. This means that a higher dose of estrogen is necessary, which may increase the risk of certain side effects. And because it’s being delivered indirectly, oral estrogen may have less of an impact on GSM symptoms. That’s why certain benefits (such as protection against UTIs) can only be obtained with vaginal estrogen.
Topical hormone therapy is an estrogen cream, gel, or spray which is absorbed through your skin. Like vaginal estrogen, this route bypasses your liver. This means your circulating estrogen level tends to be more stable, which may help prevent side effects. The downside of this method is that it can be somewhat inconvenient. You’ll have to be careful to not inadvertently wash or rub off the medication—and to not let other people (e.g. children) make contact with it.
Final thoughts
Menopause symptoms like painful sex, vaginal irritation, and urinary difficulties are not a normal part of aging that we need to accept. They’re real health issues that can take a real toll on your quality of life. Vaginal estrogen has been proven safe and effective in treating these symptoms—and it’s an increasingly important part of our modern menopause toolkit.



